by Ben Taylor
Omicron wave reaches Tanzania
The Omicron variant of Covid-19 has reached Tanzania and spread widely. This conclusion is not based on analysis of official data on case numbers, hospitalisations and deaths, but instead on anecdotal (but very widespread) reports of case numbers having risen sharply in December 2021 both in health facilities and in the community.
On November 27, the government urged Tanzanians to take all the necessary precautions to prevent the spread of the coronavirus as the new Omicron variant of the Covid-19 virus threatened to roll back the global fight against the disease. A statement issued by Tanzania’s chief medical officer, Dr Aifello Sichwale, said the fourth Covid-19 wave caused by the new variant was “deadly”.
There is still very little official data being released on the state of the pandemic in Tanzania (with the exception of data on vaccines – see below). The government has released some data – for example Situation Report No.14, dated December 20th, 2021, reported 1,366 new confirmed cases in the previous week, 92% of which were in Dar es Salaam, bringing the reported total since the start of the pandemic to 27,849, with 737 confirmed deaths. However, such releases have been highly sporadic and inconsistent. Moreover, the figures they contain are thought to be massive underestimates.
Nevertheless, in contrast to earlier phases of the pandemic, doctors and others are far more willing now to speak openly about what they are seeing. The story they tell is remarkably consistent from different parts of the country, and paints a mixed picture.
“We’re seeing a lot of patients arrive at the hospital,” said a senior doctor at Muhimbili National Hospital, “but most do not actually need to be admitted.” A doctor in Iringa said there were clear signs that the virus was spreading widely in the community – “everybody has it”, he said – but that for most people it was proving no more serious than an unpleasant flu.
The Situation Report cited above also included a revealing chart showing confirmed case numbers across the full period of the pandemic. The chart is interesting not so much for the specific figures (which are likely to be underestimates) as for the pattern of numbers rising and falling in particular periods. These waves match closely those experienced in Kenya and Uganda where data has been released regularly throughout.
Even more interesting still, however, is the fact that the chart shows case numbers from times when Tanzania was not officially collecting such data, and indeed when the government was publicly making the claim that the country had defeated the virus and was experiencing no cases.
STOP PRESS: At the time of writing, President Samia Suluhu Hassan announced a cabinet reshuffle, which returned former Minister of Health, Ummy Mwalimu, to the position, replacing Dr Dorothy Gwajima. Mwalimu had previously served as Minister of Health from 2015 to November 2020, when she was removed from the post, reportedly as a result of disagreements with the President over the national response to Covid-19.
Tanzania hits 2,000,000 Covid-19 vaccines milestone
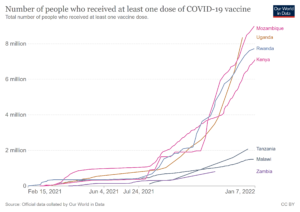
Shortly before the end of 2021, Tanzania reached the figure of two million people having received at least one dose of a vaccine against Covid-19 (3.4% of the population). This puts the country at a similar level to Zambia and Malawi, but well behind Kenya (over 7 million people vaccinated), Uganda (8 million) and Mozambique (9 million).
Tanzania started later than many other countries in providing vaccines, with the vaccine rollout not getting underway in earnest until August 2021, compared to February or March for many of the country’s neighbours.
This is a direct effect of the anti-vaccine stance of the late President John Magufuli, who had refused offers of vaccines, arguing that they did not work and could even be dangerous. President Samia Suluhu Hassan changed this position, joining the global COVAX initiative that supplies vaccines free of charge to poorer countries and accepting offers of vaccines donated by the USA and China. Between July and December, Tanzania received a total of 4.8 million doses of the Moderna, Pfizer, Johnson & Johnson and Sinopharm vaccines from various sources.
Nevertheless, the relatively slow pace of vaccination in Tanzania reflect two separate legacies of President Magufuli’s idiosyncratic response to the Coronavirus pandemic, in addition to the late start.
First, in contrast to her neighbours, health authorities and service providers in Tanzania had not been making preparations for a nationwide vaccine rollout. Nor had they shifted to pandemic-footing more generally – with no systematic monitoring of case numbers, for example, or efforts to raise public awareness of the virus. Indeed, under President Magufuli, there were concerted efforts to downplay the pandemic’s seriousness.
Second, many Tanzanian citizens who a few months earlier had heard their much-loved President tell them that the vaccines were ineffective and dangerous, are now reluctant to put their trust in those very same vaccines. A recent survey of public opinion by Twaweza , a civil society organisation working in Tanzania, Kenya and Uganda, found that just half of Tanzanian citizens (54%) would be willing to get vaccinated against Covid-19, compared to 76% in Kenya and 85% in Uganda.
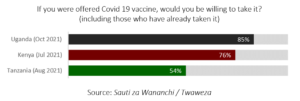
fig 3 (Source: Sauti za Wananchi, Twaweza). Disclosure: the author of this article works for Twaweza
Overcoming such resistance will not be straightforward.
Malaria vaccine approved for widespread use
The World Health Organization in October endorsed the first vaccine against Malaria, a disease that kills more than 400,000 people a year, mostly African children. The decision followed a review of data from trials of the vaccine developed by GSK, conducted since 2019 in Ghana, Kenya and Malawi in which more than two million doses were given of the vaccine.
After reviewing the evidence, the WHO said it was “recommending the broad use of the world’s first malaria vaccine”, the agency’s director general Tedros Adhanom Ghebreyesus said. The WHO said it was recommending children in sub-Saharan Africa get four doses up to the age of two.
Findings from the vaccine trials showed it “significantly reduces severe malaria which is the deadly form by 30 percent,” said Kate O’Brien, Director of WHO’s Department of Immunization, Vaccines and Biologicals. The vaccine is “feasible to deliver”, she added and “it’s also reaching the unreached… Two thirds of children who don’t sleep under a bed net in those countries are now benefiting from the vaccine.”
Many vaccines exist against viruses and bacteria but this was the first time that the WHO recommended for broad use a vaccine against a human parasite.
“From a scientific perspective this is a massive breakthrough,” said Pedro Alonso, Director of the WHO Global Malaria Programme.
The estimated cost of malaria in sub-Saharan Africa is over 12 billion dollars a year, Alonso said at a news conference following the announcement. The GAVI vaccine alliance said they will consider whether and how to finance a new malaria vaccination programme for countries in sub-Saharan Africa.
The WHO also hopes this latest recommendation will encourage scientists to develop more malaria vaccines.
Separately, the fight against malaria earlier in 2021 received a major boost when researchers from Britain’s Oxford University announced that their Matrix-M vaccine candidate had become the first to surpass the WHO’s threshold of 75-percent efficacy. Germany’s BioNTech, which developed a coronavirus vaccine with US giant Pfizer, also said it aimed to start trials for a malaria vaccine next year using the same breakthrough mRNA technology.
The Oxford team launched a phase-3 trial in summer 2021, enrolling 4,800 children in Burkina Faso, Mali, Kenya and Tanzania. If all goes as hoped, results could be submitted to regulators in late 2022.
Adrian Hill, Director of the Jenner Institute at the University of Oxford said that “in Africa, malaria has probably caused four times as many deaths as COVID-19 over the past year”.